Cervical cancer in light of comprehensive care!
Writers: Ms Zaakya Al Habsi, Clinical Nurse Specialist- Dr Sarya Bella, Gynecological Oncologist – Dr Ana Paula Gozales-Lopez, Radiation Oncologist – Dr Aref Zribi, Medical Oncologist- Dr Ikram Burney, Medical Oncologist
Management of Gynaecological Cancers across the continuum of care – Part 7
Worldwide, January is observed as Cervical Cancer Awareness Month. It is an excellent opportunity for the staff of Women Health Program at SQCCCRC to write a few lines to raise awareness about cancer of the cervix amongst community in Oman. Cervical cancer is preventable, while it develops, it can be detected early through screening, and if diagnosed, is one of the most treatable cancers, provided it is detected early and managed effectively. Cancers diagnosed in late stages can also be controlled with appropriate treatment and palliative care. Generally, the public is not aware of the scientific and medical developments in prevention, screening, and management of cervical cancer, hence, this article is intended to increase awareness about these aspects of cervical cancer.
Epidemiology:
Cancer of the Uterine Cervix is the 4th most common cancer amongst women in the world. More than half-a-million new cases of cancer of cervix are registered every year, and almost 250,000 patients die of the disease. The incidence and mortality of cancer of cervix is highest in the developing world. In the Eastern Mediterranean Region (EMRO), cancer of cervix is the 6th most common cancer in women. Annually, around 90,000 women are diagnosed and around 50,000 die of the disease in the EMRO region. In Oman, around 30-35 new cases are registered every year. However, almost 1/3rd of the patients present with widespread disease (stage IV). Cancer of cervix lends itself to both primary (general population), and secondary (high risk patients individuals) prevention, and this has been shown to reduce the mortality.
Prevention and Early Detection:
Primary prevention is based on awareness and education of the general population on risk factors. Human Papilloma Virus (HPV) is recognized as the most important causative factor and accounts for almost 99% of all cancers of the cervix. The virus is transmitted during sexual intercourse. Limiting the number of sexual partners, and HPV vaccine have been shown to reduce the risk significantly. The vaccine should be given ideally as two doses, 6-months apart, to girls, before their first sexual experience. For secondary prevention of cancer of cervix, screening is done using Papanicolaou Test (Pap smear). The Pap test has been the standard method for detecting the cancer early, hence reducing the incidence of invasive cancer by 60%–90% and the death rate by 90%. More recently, screening is based on detection of the virus directly from the specimens obtained from the cervix.
Diagnosis and Clinical Staging:
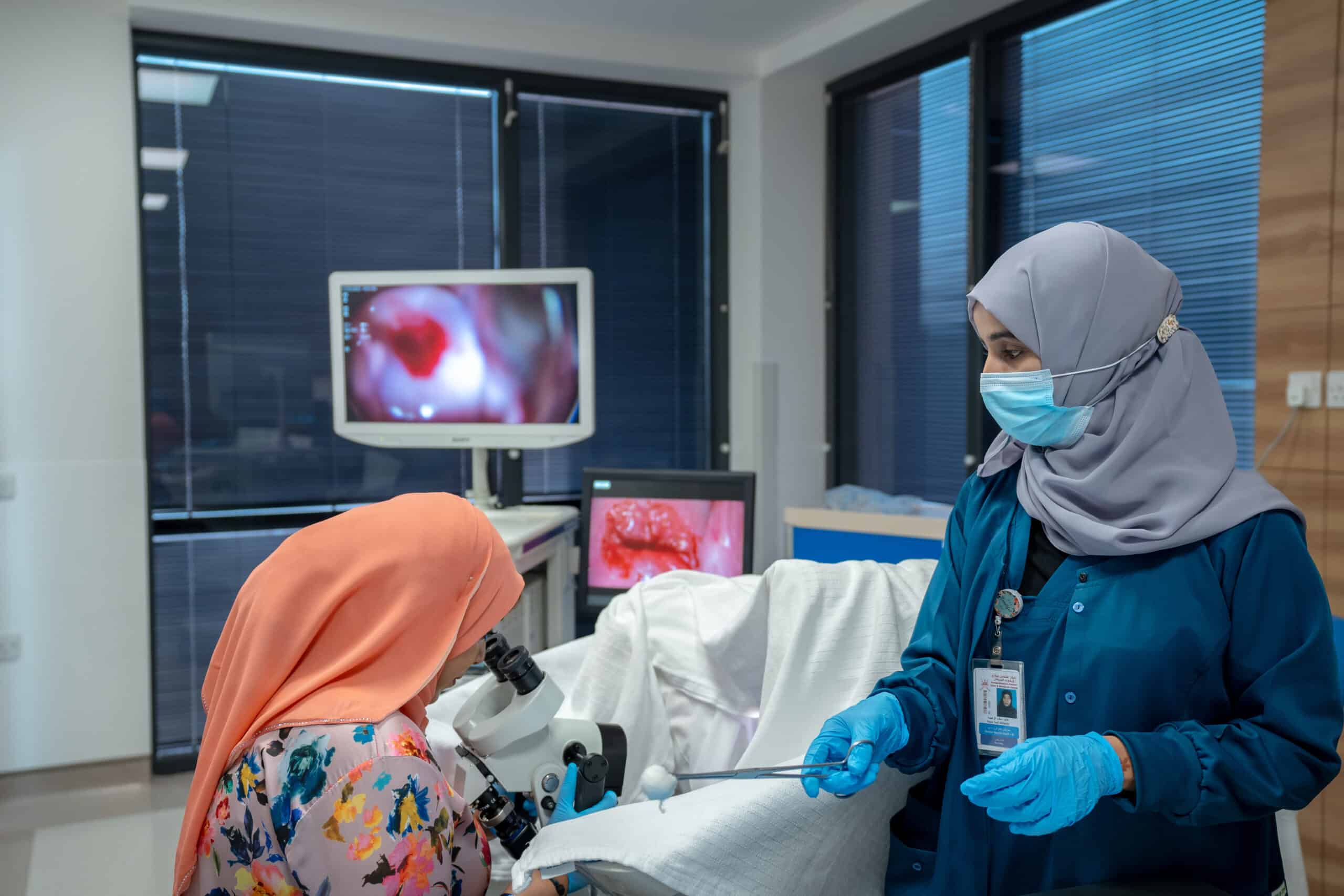
Once the cancer is suspected, the patient should undergo a specific test in the out-patient gynecology clinic, called colposcopy, where a biopsy is obtained. There are several types of cervical cancer; more than 70% are squamous cell carcinoma. Once the diagnosis is established, a detailed physical examination, an MRI of the pelvis, and a chest x-ray will be done to know the extent of the disease. If the cancer is suspected to be locally advanced, then a PET-CT scan is done to study the extent of spread of cancer (clinical staging).
Management planning:
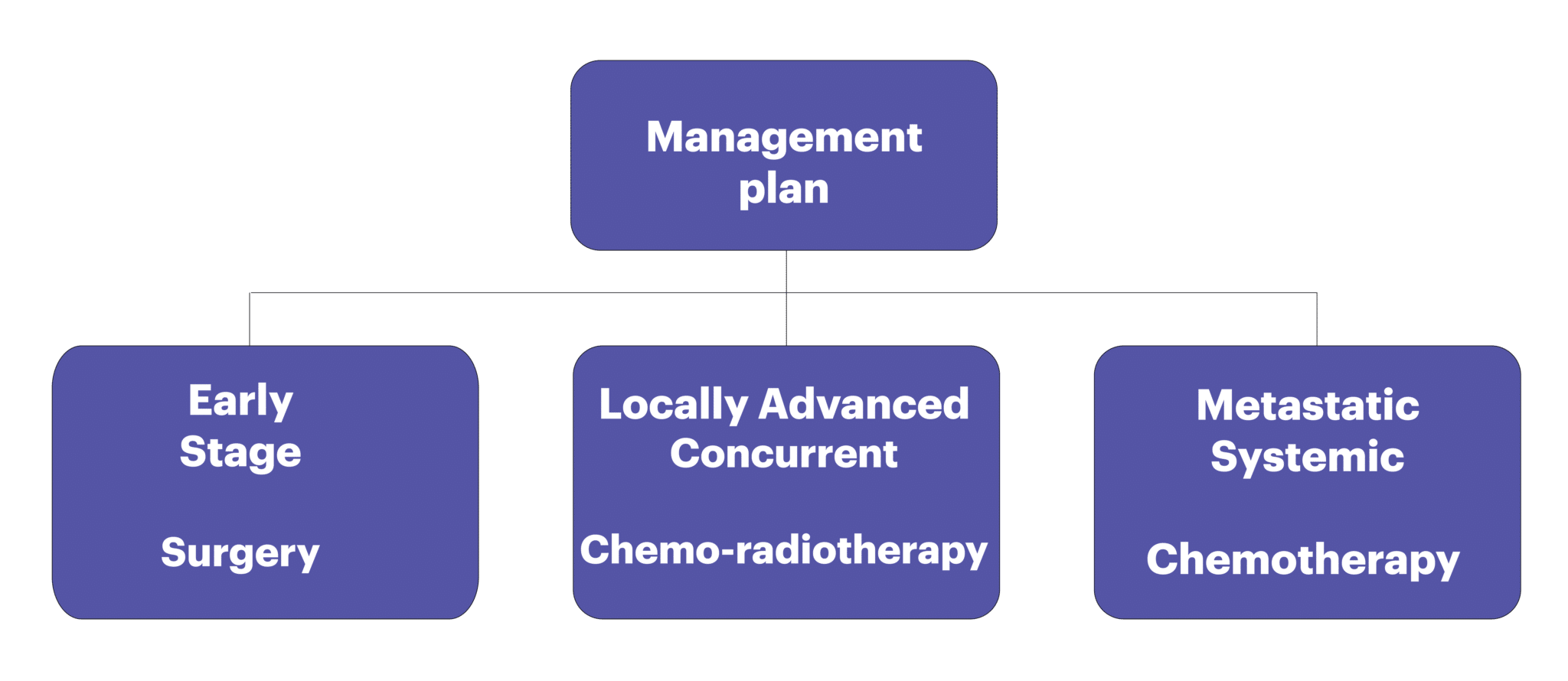
Each patient’s case is discussed in a muti-disciplinary meeting (tumor board, where the biopsy results are explained by the pathologist and reviewed by members of the board, and all radiological investigations are explained by the radiologist, and reviewed by all present). Following a discussion between the surgeons, radiotherapists, and the medical oncologists, a plan of action is formulated for each individual patient, considering other factors, such as age, other illnesses, and patient’s preferences. Further management depends on the clinical stage as follows:
Surgery:
Complete removal of the uterus (hysterectomy) is the treatment of choice if the patient does not wish to preserve fertility. If the disease is more than 2 cm, a radical hysterectomy is the standard treatment. A significant number of women with early cervical cancer are diagnosed to have cancer of cervix during reproductive age and may wish to remain fertile. These patients demand a more conservative policy for the management of cancer. A very early-stage cancer can be managed with conization or simple trachelectomy.
Radiotherapy:
Radiotherapy plays an important role in the management of cervical cancers. This form of treatment utilizes high-energy X-rays to damage cancerous cells. It has been proven to be highly effective when the disease is locally advanced. The advantage of radiotherapy is its ability to deliver high doses of radiation to the tumor while sparing the healthy organs around the cancerous area. This is essential for cancer of cervix as it is located near critical structures such as the urinary bladder and the rectum. Radiotherapy can be delivered in 2 forms:
- External beam radiation therapy delivers treatment to the tumor from a machine outside of the body, called linear accelerator. Treatment is administered 5 days a week for 5 weeks, and each session lasts approximately 25 to 30 minutes. The total number of sessions depends on the treatment assigned by the radiation oncologist. During radiotherapy, chemotherapy is also administered once a week every week for 5 weeks. This enhances the effect of radiotherapy. The combination treatment is also called concomitant chemo-radiotherapy or CCRT.
- Brachytherapy is a form of internal radiation therapy that involves the placement of radioactive sources inside or near the tumor, allowing high doses of radiation to be delivered precisely to the affected area. Brachytherapy is administered after the CCRT.
Before the radiotherapy treatment starts, the radiation oncologist arranges a CT scan, or an MRI, or both, to plan the appropriate dose and volume of treatment for each individual and explain the possible side effects.
Systemic therapy:
If the disease is widespread at the time of diagnosis (about 1/3rd of all patients in Oman), chemotherapy is administered to control the disease. As a result of recent advances, more than 80% of the patients would receive a 4-drug combination, which is delivered all in one day, in the day care unit. The combination consists of 2 types of chemotherapy, a drug which prevents blood vessels formation feeding the tumor, and an immune checkpoint inhibitor, which allows the body’s immune system to fight against cancer. More than 50% of the patients will respond to this combination, and the cancer shrinks. In such a case, 1st three type of drugs are stopped after 6 cycles, and the immune checkpoint inhibitors are continued for at least two years; sometimes longer.
Treatment at relapse:
If the disease persists or recurs after surgery or radiotherapy, or first round of chemotherapy, the patient is evaluated for further treatment, and this could consist of surgery, however, for most patients, a 2nd type of chemotherapy is administered to try and control the disease.
Holistic care:
At the SQCCCRC, all patients diagnosed with cancer of cervix, or any other cancer, receive holistic care. Patient’s psychological wellbeing is addressed, and all patients are assessed for mood changes, such as anxiety and depression. If needed, a psychologist or a psychiatrist will see the patient at the same time as the surgeon, radiation, or the medical oncologist. In addition, a clinical nutritionist, a physiotherapist, and a clinical pharmacist will assess the patient’s needs and provide appropriate support. Patients or their immediate family members have access to the clinical nurse specialist through phone and WhatsApp message.