What do you know about thyroid cancer?
Article: Dr.Omayma Elshafie – Senior Consultant Endocrinology
Introduction:
Thyroid follicular epithelial-derived cancers include papillary, follicular, and anaplastic cancer. Papillary and follicular cancers are considered differentiated cancers, and patients with these tumors are often treated similarly despite numerous biologic differences.
Incidence:
In a report based upon the Surveillance, Epidemiology, and End Results (SEER) database from 1975 to 2018, the incidence of papillary cancer increased from 4.8 to 14.9 per 100,000.
The increase in incidence of thyroid cancer is due to increase in imaging use, such as CT scan, MRI and Ultrasound.
Risk Factors:
-Radiation exposure — Radiation exposure of the thyroid during childhood
-Family history — A history of thyroid cancer in a first-degree relative or a family history of a thyroid cancer syndrome
-Older than 40 years of age
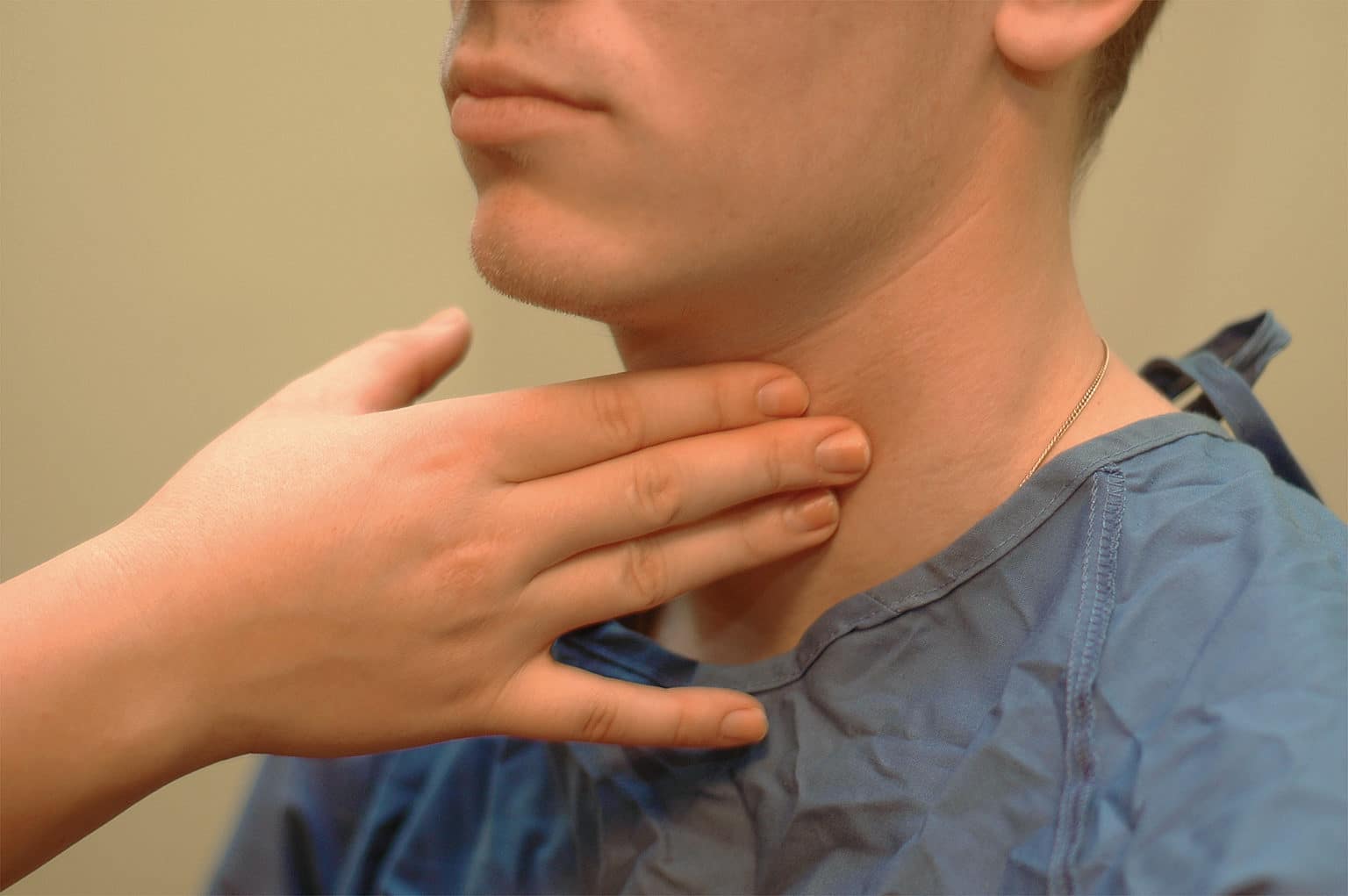
Clinical features:
Clinical presentation — Thyroid cancer typically presents as a thyroid nodule. Thyroid nodules come to clinical attention when noted by the patient; during routine physical examination; or when incidentally noted during a radiologic procedure, such as carotid ultrasonography, neck computed tomography (CT), magnetic resonance imaging (MRI), or positron emission tomography (PET) scanning.
Types of thyroid cancer:
1.Papillary thyroid cancer. Most common
2.Follicular thyroid cancer
3.Medullary thyroid cancer
4.Anaplastic thyroid cancer
Spread of the disease:
From 2 to 10 percent of patients have metastases beyond the neck at the time of diagnosis. Among such patients, two-thirds have pulmonary and one-fourth have skeletal metastases. Rarer sites of metastasis are the brain, kidneys, liver, and adrenals.
Prognostic Features:
Most patients with papillary cancer do not die of their disease and have a normal life span.
The mortality of thyroid cancer increases with advancing age, tumor size and presence of metastasis
Treatment:
Surgery
The first step in treatment for all types of thyroid cancer is surgery which is the best chance at cure. The key is a good surgeon.
Radioactive iodine therapy (Also referred to as I-131 therapy)
Thyroid cells and most differentiated thyroid cancers absorb iodine so radioactive iodine can be used to eliminate all remaining normal thyroid tissue and potentially destroy residual cancerous thyroid tissue after thyroidectomy
Follow up
Periodic follow-up examinations are essential for all patients with thyroid cancer with physical examination, thyroid cancer markers (thyroglobulin) and ultrasound thyroid to assess for recurrence of disease. Thyroid function test to adjust hormone level based on patient’s risk. Follow up is done every 6 to 12 months.