How to protect yourself from gynecological cancer?
Author: Dr. Ikram Burney – Senior Consultant in Medical Oncology and the lead for the Gynecological Oncology Program
Management of gynecological Cancers across the continuum of care – Part 1
This is first of a series of several articles intended to increase awareness about cancers of the female genital tract. Management of cancer can be seen across the continuum of care, from prevention, early detection, diagnosis, treatment and symptom management through survivorship.
In this article, methods of prevention of gynecological cancer are described. Measure for prevention of cancer can be described as:
- Primary prevention, (applicable to all individuals)
- Secondary prevention (applicable to people at high risk of getting the cancer).
- Tertiary prevention, (prevention of cancer once the cancer is successfully treated).
According to data from the Globocan, cancers of the female genital track are the 5th most common cause of cancer worldwide, after cancers of the lung, breast, colon and prostate. The three most common forms of gynecological cancers include cancers of the uterine cervix, uterus and the ovaries. Cancer of the uterine cervix is the 3rd most common cause of cancer in women. Around half-a-million patients are diagnosed to have the cancer annually. However, there is a huge geographic variation. In some countries, cancer of the uterine cervix is the most common cancer. Cancer of the uterus is the 6th most common cause of cancer worldwide, and the most common form of gynecological cancer in the western world. Cancer of the ovaries is the 8th most common cause of cancer in women worldwide.
The National Cancer registry of Oman reports the incidence of cancer annually. The latest data on incidence and the pattern of increase over the years are shown in the figure below:
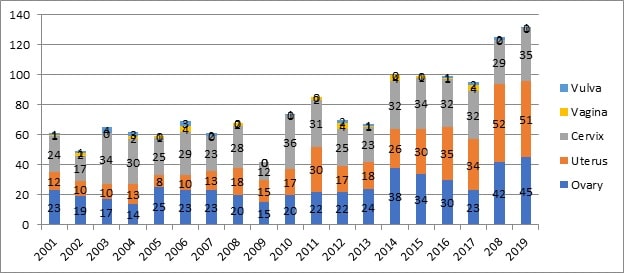
Source: Cancer Incidence in Oman 2019. Department of non-communicable diseases, Directorate General of Primary Health Care
Evidence-based measures for primary prevention of cancer have been described by the World Cancer Research Fund (WCRF), and the American Institute for Cancer Research (details can be accessed at wcrf.org). The preventive measures described below apply to all other forms of cancers and are intended for the general public. The measures include.
Lifestyle measures:
- Exercise, (150 to 300 minutes every week). Exercise includes brisk walking, running, jogging, swimming, and active gardening.
- Maintaining the body mass index close to normal (25kg/m2). Body mass index can be calculated by using smart phone Apps. Alternatively, BMI can be calculated by dividing weight (kg) by square of height (meters).
- Not smoking or quitting smoking.
- Not drinking alcohol.
Eating prudently:
- Consuming fresh fruits, green vegetables, and brown bread (5/15 portions every day).
- Restricting the intake of red meat (5 portions in a week).
- Restricting the intake of preserved and processed food.
- Restricting the intake of high energy drinks.
- Not using the supplements for prevention of cancer. However, replacing the deficiency of nutrient, such as, vitamin D, is permissible.
Breastfeeding
- solely till the age of six months, and then weaning.
Several prospective studies, including the ViTals and the EPIC studies, involving hundreds of thousands of individuals, followed up longitudinally, have shown that individuals who follow the vast majority of recommendations have a 30% lower risk of developing cancer, compared to those who follow only a few of these recommendations.
In addition, for primary prevention of the cancer of the uterine cervix, the IARC recommends the administration of Human Papilloma Virus (HPV) vaccine before the girls start sexual activity. Two doses of the vaccine should be administered with an interval of 6-15 months.
Secondary prevention would be described for the three common gynecological cancers separately.
Cancer of the uterine cervix.
Secondary prevention is aimed to decrease the incidence and prevalence of cervical cancer by screening all women aged 30-49 years, every five years. If two consecutive tests are negative, then the screening frequency could be reduced to once every 10 years. Various methods are available; testing for HPV DNA is the gold-standard. If a precancerous lesion is identified, then it should be treated.
Cancer of the uterus.
The mainstay of secondary prevention for uterine cancer is prevention and treatment of obesity. 80% of patients diagnosed to have cancer of the uterus are obese (BMI > 30kg/m2) at the time of diagnosis, and several patients have concomitant high blood pressure, diabetes mellitus and hyperlipidemia. Compared to women whose weight is normal, Obese women have a 3-fold higher risk of developing uterine cancer; the risk increase to 7-fold if the BMI is more than 40kg/m2.
Additionally, women who have a family history of uterine or colon cancer should undergo genetic test. If a genetic defect is identified, the risk of getting uterine cancer may be as high as 50-60% over the course of lifetime. High-risk individuals should undergo annual screening, beginning at the age of 35, and may be offered prophylactic hysterectomy once they complete their family life.
Cancer of the ovary.
Women who have a family history of breast or ovarian cancer, should undergo genetic testing. If a mutation is found in BRCA1 or the BRCA2 gene, the risk of getting a diagnosis of ovarian cancer over the lifetime is 45% and 12% respectively. The risk of getting breast cancer during the lifetime is also very high. Such individuals need discussion with their doctors, who might suggest risk-reducing bilateral salpingo-oophorectomy (removal of both ovaries and the fallopian tubes) after the individuals do not wish to have more children. The procedure can reduce the risk of ovarian cancer by more than 80%.
Patients diagnosed to have cancer should be treated with standard-of-care and undergo regular screening for tertiary prevention. In addition, the patients should observe all measures suggested for primary prevention.
The details of the screening methods for the gynecological cancers would be discussed in the next issue