Physiotherapy Improves the Quality of Life of Cancer Survivors: A Case Study.
Writers: Samiya Marhoon Salim Al Kalbani- Physiotherapist/ Dr. Ikram A Burney- Senior Consultant Medical Oncology, Head of Women’s Health Program
Management of gynaecological cancers require integrated multi-disciplinary care. Besides the gynaecological, medical and radiation oncologists, multidisciplinary management requires clinical nurse specialists, geneticists and counsellors, psychiatrists, palliative care specialists, clinical pharmacists, clinical nutritionists, and physiotherapists. Using the case study of a patient who underwent treatment at the SQCCCRC, we write to highlight the role and importance of integrating physiotherapy in the overall management of patients with gynaecological cancers.
Case description and evaluation:
A 45-year-old lady presented to the Cancer Center with a history of foul-smelling vaginal discharge. Previously, MRI had shown a large mass measuring 17 x 9.8 x 4.7 cm pelvic mass infiltrating the urinary bladder, and a CT scan showed bilateral hydronephrosis, and bilateral pulmonary metastases. Biopsy of the mass protruding into the urinary bladder revealed a diagnosis of uterine sarcoma. She had undergone total abdominal hysterectomy 10 years back for fibroids.
The patient was admitted to the in-patient ward. She was brought on a wheelchair. She looked unwell, had high grade fever, was tachycardic and hypotensive. She was barely able to mobilize and was not able to carry out the activities of daily living. Initial physiotherapy evaluation included chest examination, muscle power assessment, range of motion in upper and lower limbs, and assessment of functional mobility including in-and-out of bed mobility. The patient was assessed functionally on the bed due to discomfort secondary to insertion of Foley’s catheter. The patient complained of burning pain around the site of foley catheter insertion which increased with movement, and heaviness in the lower limbs. A hard mass, likely arising from the pelvis, was palpable on abdominal examination. She had mild oedema in both hands, swelling near perineal area, along with lower limb oedema, reduced muscle power in both upper and lower limbs, was able to walk with assistance, but with a moderate risk of fall, and limited mobility due to pain and fatigue.
Physiotherapy role in improving patient’s quality of life:
During the course of admission, the patient received physiotherapy sessions on a daily basis, including out-of-bed mobilization, balance exercises, lower and upper limbs exercise (range of motion, endurance and strengthening exercises) with progression in types of exercise and frequency. After 16 days, the patient was discharged with good health condition and physical performance. She was able to walk independently with good balance. Both fatigue, and oedema had improved. Home physiotherapy program was given, so that the patient could continue same exercises at home. The patient followed up in the Day Care Unit to receive palliative chemotherapy, gemcitabine, and docetaxel in standard doses, where she was evaluated regularly.
During the course of palliative chemotherapy, the patient was admitted to the in-patient wards four more times, due to repeated infections of the urinary tract and over the tumor site. On at least two occasions, the reason for admission was sepsis, and acute kidney injury. The lower limb edema re-occurred in the upper portion of left thigh with tenderness. It caused muscle weakness, difficulty in mobility (in-and-out of bed). Patient’s mobility state and functional activities deteriorated. However, following repeated physiotherapy sessions, the patient was able to sit up from lying position, turn in the bed with minimal support, stand up and walk a few steps with moderate level of assistance and fair dynamic balance, but got fatigued easily after walking short distances. Over the course of admission due to sepsis, she stayed for 37 days and received physiotherapy sessions daily including in-and-out of bed mobility, lower limb therapeutic exercises, balance training, muscle strengthening exercises and energy conservation education. She improved gradually along with the treatment of the underlying cancer. By the time she was to be discharged home, she was able to sit, stand and walk independently with less fatiguability.
The patient was admitted a couple of times afterwards for repeated urinary tract infections, or infection at the percutaneous nephrostomy site, and was managed with antibiotics and ongoing physiotherapy sessions.
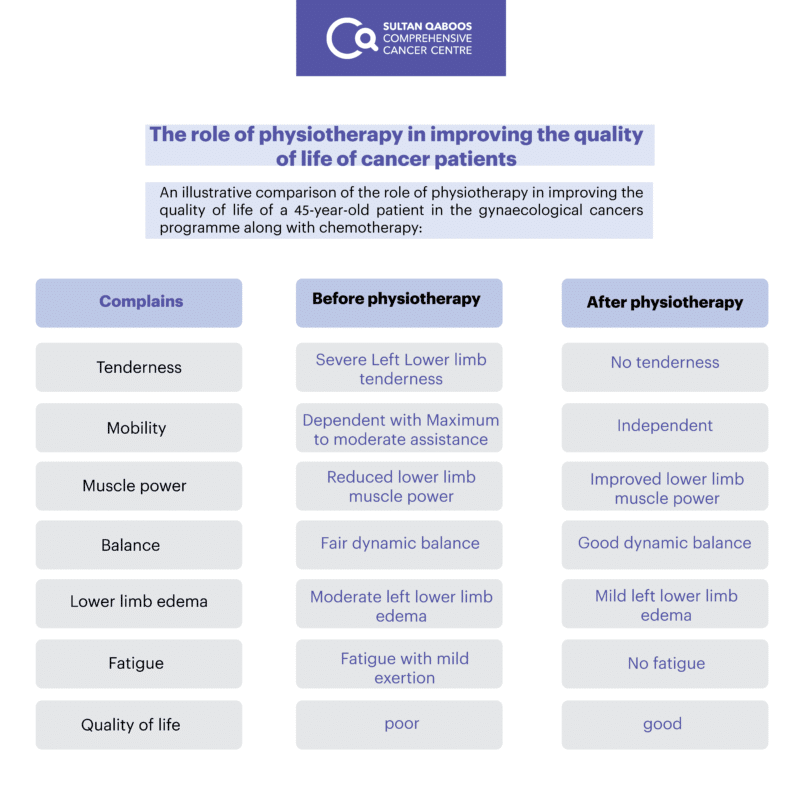
End of physiotherapy and chemotherapy course of the case:
Towards the end of the course of treatment with palliative chemotherapy (six months), the patient had significant improvement in functional activities. She reported carrying out household chores, including gardening, walking at home independently, and carrying out regular exercises. On examination, she was able to walk independently for long distances with good static and dynamic standing balance and had good muscles power except for left iliopsoas muscle. She still has lower limb edema but much less than before. Generally, the patient was more satisfied in her current state, as she was independent in mobilization and did not feel fatigued.
Conclusion:
To summarize, the patient was admitted to the in-patient ward five times over the course of six months, once even up to 37 days, and received 12 doses of palliative chemotherapy in the Day Care Unit. In addition to the systemic cytotoxic treatment, and supportive care, she received physiotherapy sessions regularly. A significant improvement was observed in the patient’s quality of life. She was able to perform activities of daily living smoothly such as cooking, showering, cleaning, walking long distance. She became fully independent in mobility with good balance in sitting and standing and did not feel fatigued while walking.
From being bed-ridden at the time of diagnosis due to progressive metastatic disease, the patient reached a stage where she could participate actively in different daily tasks at the end of the treatment. During the 6-month course of treatment, the underlying metastatic uterine sarcoma remained stable as seen on the radiological assessment, but her performance status improved from 4 to 1 on the World Health Organization (WHO) scale. Such was the transformative effect of physiotherapy, that we chose to present the details of treatment and care as a case study. The case study not only highlights the role and importance of physiotherapy, but also emphasizes the importance of holistic care. Physiotherapy utilizes movement science to help individuals to maintain and maximize their physical strength, range of motion, and functional and overall well-being. Through these measures, physiotherapy improves the quality of life of patients with gynecological cancers. Physiotherapists should be part of the team delivering integrated, holistic care to patients with gynecological cancers, and should participate and contribute to the multi-disciplinary tumor boards.






